HPV and cervical cancer: facts and perspective
An HPV diagnosis causes fear of cervical cancer. But HPV does not equal cancer. The process from HPV to cancer takes years and offers the opportunity to intervene at any time.
HPV does not equal cancer
The fear is understandable. You have HPV, and the first thing you think of is cervical cancer. But it is important to know the facts and maintain perspective. HPV is incredibly common and, in the vast majority of cases, does not lead to cancer.
of all women will contract HPV at some point. It is one of the most common viral infections in the world. In most women, the immune system clears the virus without it ever causing symptoms.
Of the women who contract HPV, only a small percentage ever develop cervical cancer. It is often a long-term process with several intermediate stages, where intervention is possible at every point.
Cervical cancer in the Netherlands: the figures
Cervical cancer statistics Netherlands (2018)
| Data | Number |
|---|---|
| New cases of cervical cancer | 830 |
| Peak age | 30-35 years |
| Trend since 2013 | Increasing |
| Women invited for national screening | 799.173 |
| Screening participation | 460.518 (< 60%) |
| Positive HPV test among participants | 32.4% |
| Referrals to gynecologist | ~14.000 |
In 2018, 830 new cases of cervical cancer were diagnosed in the Netherlands. The peak age is between 30 and 35, and an upward trend has been visible since 2013.
In 2024, more than 900 women were diagnosed with cervical cancer.
After reaching a low point in 2013, the total number of women with cervical cancer has risen again. Young women with cervical cancer often turn out not to have been vaccinated with the HPV vaccine.
Of the nearly 800,000 women invited for the national screening program, less than 60% participated. Among the participants, 32.4% tested positive for HPV, leading to approximately 14,000 referrals to the gynecologist.
These figures underline two things: HPV is very common, and regular screening is essential for early detection.
From HPV to cancer: often a long-term process
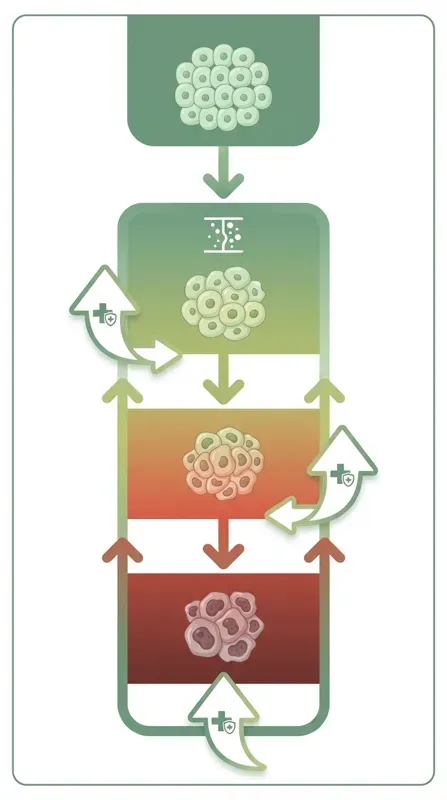
Cervical cancer does not develop overnight. It is a process that takes years. This provides a crucial window of opportunity to intervene.
The process from HPV to cervical cancer
HPV infection
The HPV virus infects the cells of the cervix. In 80-85% of women, the immune system clears the virus within 2 years. No action is needed, but monitoring is wise.
Persistent infection (15-20%)
In 15-20% of women, the virus remains present for longer than 2 years. The virus can integrate its DNA into the host cell and activate the E6/E7 oncogenes. This is the moment to actively intervene.
Mild abnormalities (CIN 1)
The virus causes superficial cellular abnormalities in the lower third of the epithelium. The majority recover spontaneously, but monitoring and active immune system support are important.
Moderate abnormalities (CIN 2)
The abnormalities extend to two-thirds of the epithelium. The chance of spontaneous recovery decreases. Treatment is considered.
Severe abnormalities (CIN 3)
The abnormal cells cover the full thickness of the epithelium but have not yet grown into the underlying tissue. Treatment is necessary.
Invasive carcinoma
Abnormal cells grow through the basement membrane into the underlying tissue. This is cancer. This stage can be prevented with timely detection and treatment in earlier stages.
is how long it takes for an HPV infection to potentially develop into cervical cancer. This process offers ample opportunity to intervene.
National screening: important but not perfect
The Dutch national cervical cancer screening program is an important tool for early detection. However, it also has limitations:
- Participation is too low: Less than 60% of invited women participate. This means more than 300,000 women per round are not screened.
- The standard HPV test is limited: The Aptima test only provides a positive/negative result, without genotyping or viral load measurement. Low concentrations of HPV can be missed.
- Long intervals: If you test negative for HPV, you are only invited again after 5 years. During that period, an infection can develop.
- No active treatment plan: In the event of a positive test, you are referred, but there is no structured program for strengthening the immune system or actively addressing the infection.
This does not mean you should skip the national screening; on the contrary, participation is important. But it emphasizes the importance of additional diagnostics and an active approach.
What can you do to prevent cervical cancer?
The good news is that cervical cancer is largely preventable. The long development process offers multiple points of intervention:
- Participate in national screening: Regular screening is the foundation for early detection
- Get comprehensive testing if HPV positive: A quantitative test provides additional information, especially as the process continues.
- Actively strengthen your immune system: Nutrition, supplements, and lifestyle influence your ability to clear HPV
- Eliminate risk factors: Quit smoking, reconsider long-term pill use, and reduce chronic stress
- Treat abnormalities promptly: Do not wait too long in cases of persistent HPV or progressive abnormalities
- Involve your partner: Prevent reinfection by also testing the male partner
Do you want to work actively on preventing cervical cancer?
At HPV Health, we help you with comprehensive diagnostics, a customized treatment plan, and continuous monitoring. Don't wait and see; take control of your health.
Schedule an intake consultationVeelgestelde vragen
How likely is it that HPV will lead to cervical cancer?
At what age is cervical cancer most common?
Why do fewer than 60% participate in the national screening?
Can cervical cancer be prevented?
Is cervical cancer hereditary?
Questions about your situation?
Feel free to get in touch for personal advice about your HPV diagnosis.
Contact us