Does smoking affect HPV?
Yes. Smoking increases the risk of serious cellular abnormalities and cervical cancer in HPV-positive women by a factor of 2.5. Quitting smoking is one of the most effective steps you can take.
Smoking and HPV: the direct link
Cigarette smoke contains more than 4000 toxic substances, more than 40 of which are carcinogenic. These include tar, nicotine, carbon monoxide, benzene, and arsenic. These substances do not just end up in your lungs; they spread throughout your entire body via the blood, including the cervix.
Research shows that smoking increases the risk of CIN 3 and cervical cancer by a factor of 2.5 (Wang et al.). This is no small difference: it means that smokers are more than twice as likely to develop serious cellular abnormalities than non-smokers.
Furthermore, there is a clear dose-effect relationship: the more you smoke and the longer you smoke, the greater the risk. Every cigarette contributes to the problem.
increased risk of CIN 3 and cervical cancer in smokers. There is a clear dose-effect relationship: smoking more and for longer results in a higher risk.
Bron: Wang et al.
How smoking exacerbates HPV
Smoking affects HPV on multiple levels simultaneously. It is not only bad for your general health; it specifically makes the HPV virus more active and your immunity specifically weaker.
1. Oxidative stress
Smoking causes an excess of reactive oxygen species in the cells. This leads to oxidative stress: a state in which free radicals damage the cells. Due to this oxidative stress, vitamin levels in the body are lowered, including vitamin C, folate, and beta-carotene—substances that are essential for defense against HPV.
2. The virus becomes more active
A 2014 study showed that smoking increases the activity of the viral proteins E6 and E7. These are precisely the proteins the HPV virus uses to cause cells to become abnormal. Simultaneously, smoking suppresses the protective p53 protein, a tumor suppressor that normally clears damaged cells.
3. CYP450 enzymes are affected
Smoking affects the enzymes CYP1A1 and CYP1A2, which are involved in estrogen metabolism and the processing of carcinogenic substances. This disrupts the balance in the cervical tissue and increases susceptibility to cellular abnormalities.
4. Vitamin deficiencies
Smoking lowers folate and increases homocysteine, a combination that reduces DNA repair and increases the risk of cellular abnormalities. Additionally, smokers tend to have low vitamin B12 levels, further disrupting cell division.
Smoking suppresses your immune system
In addition to the direct effects on the virus, smoking also impacts the immune system on several fronts:
- Type 1 interferons are inhibited: These are antiviral cytokines that play a crucial role in the first line of defense against viral infections. Smoking suppresses their production.
- TH1 cells are reduced in the airways: TH1 cells are essential for the cellular immune response against viruses. Smoking reduces their number and function.
- T-lymphocytes are compromised: T-lymphocytes are crucial for the elimination of HPV. They recognize and destroy infected cells. Smoking affects both the number and the function of these cells.
The result: your body is less able to clear the HPV virus, causing the virus to remain present longer and increasing the chance of progression to more serious cellular abnormalities.
Quitting smoking helps
The good news: quitting smoking demonstrably helps. Research shows that after quitting smoking, the severity of CIN abnormalities can decrease. Your immune system gradually recovers, and your body gets the chance to fight the HPV virus effectively again.
This makes quitting smoking one of the most concrete and effective steps you can take as an HPV-positive woman — alongside nutritional optimization and immune system strengthening.
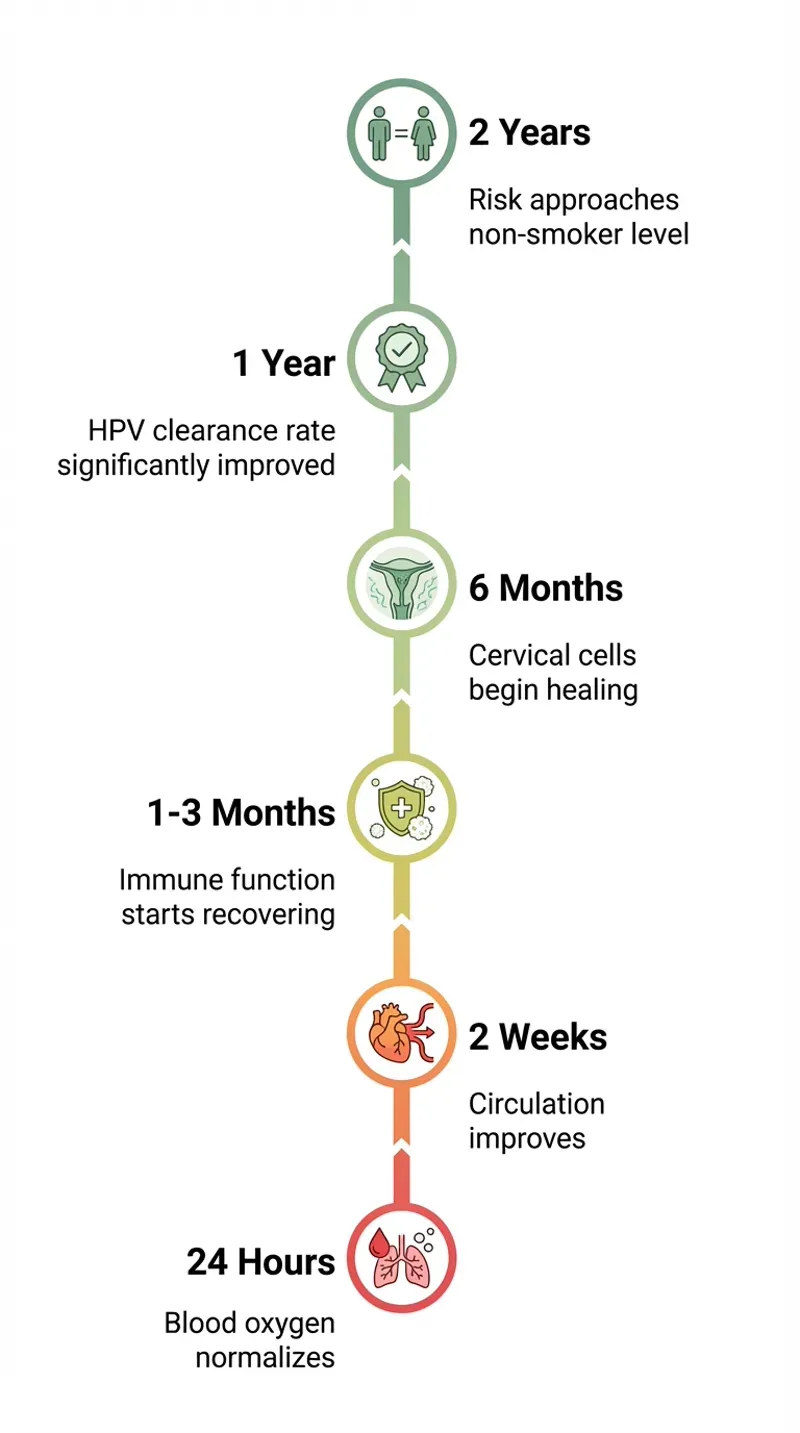
What happens when you quit?
First weeks: vitamin levels recover
Levels of vitamin C, folate, and B12 begin to normalize. Oxidative stress decreases and cells experience less damage.
1-3 months: immune system recovers
T-lymphocytes and interferons begin to recover. The immune system becomes more effective again at recognizing and fighting HPV-infected cells.
3-6 months: measurable improvement
After a few months, a decrease in the severity of CIN abnormalities can be observed. The chance of HPV clearance increases.
In the long term: risk drops significantly
The increased risk of cervical cancer gradually decreases. The sooner you quit, the greater the benefit.
Support with quitting and HPV treatment
Quitting smoking is an important part of our treatment advice. During the intake consultation, we discuss how we can support you in this, alongside targeted HPV treatment.
Contact us