Is the contraceptive pill a risk factor for HPV?
Yes. Long-term use of the contraceptive pill (longer than 5 years) can increase the risk of abnormal cells and cervical cancer. The pill itself does not cause HPV! The use of the contraceptive pill is associated with a higher occurrence of ectropion at the cervix. Estrogen processing also appears to have an influence and is a complex process.
Estrogens and their influence on cell changes in sensitive cells
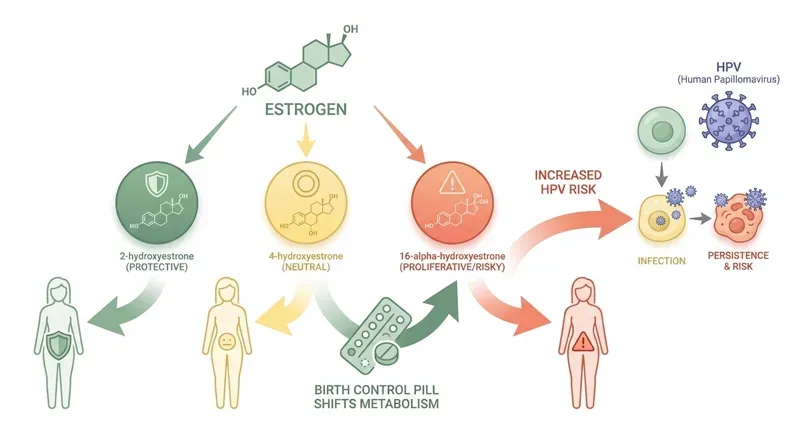
To understand why the pill is a risk factor for HPV, you need to know how estrogen metabolism works. Estrogen is broken down in your body via the CYP450 system in the liver. This produces three different metabolites, each with a different effect:
- 2-hydroxy-estrone: The "good" metabolite. This variant has a protective effect and is associated with a lower risk of cell abnormalities.
- 4-hydroxy-estrone: Associated with tumor growth. This metabolite can cause DNA damage and promote the development of abnormal cells.
- 16a-hydroxy-estrone: Associated with DNA damage. This metabolite binds irreversibly to the estrogen receptor and can stimulate cell proliferation.
The enzymes CYP1A1 and CYP2E1 are involved in this process and are specifically associated with cervical neoplasia. When estrogen metabolism shifts toward the harmful pathways (4-OH and 16a-OH), the risk of cell abnormalities increases.
Estrogen metabolites compared
| Metabolite | Classification | Effect | Influenced by |
|---|---|---|---|
| 2-hydroxy-estrone | Favorable | Protective effect, lower risk of cell abnormalities | DIM/I3C from cruciferous vegetables |
| 4-hydroxy-estrone | Unfavorable | Promotes tumor growth, causes DNA damage | Genetic variations (CYP1A1) |
| 16a-hydroxy-estrone | Unfavorable | Binds irreversibly to receptor, stimulates cell growth | Long-term pill use, obesity |
The pill as a cofactor for HPV
The direct link between the pill and HPV lies in the E7 protein. This is one of the two viral proteins (along with E6) responsible for cell derailment. E7 requires estrogen as a cofactor to function effectively.
In concrete terms: estrogen suppresses the tumor suppressor genes p53 and pRb. These genes are normally the guardians of your cells: they ensure that damaged cells are repaired or cleared away. When estrogen suppresses these genes, the E7 protein can operate undisturbed.
The danger arises when highly oncogenic types persist, particularly HPV 16. On a cellular level, the oncoproteins E6 and E7 play a key role by disrupting the function of anti-tumor defense proteins.
Long-term pill use
Research shows that with the use of oral contraceptives (OCs) for longer than 5 years, the risk of abnormal cells and cervical cancer is increased. This risk increases with the duration of use.
It is important to emphasize that the pill itself does not cause cervical cancer. The increased risk specifically applies to women who are also HPV-positive. It is the combination of HPV infection and long-term estrogen use that increases the risk.
This does not mean that every woman who uses the pill and is HPV-positive will develop cell abnormalities. But it is a factor to consider, especially when CIN abnormalities are already present.
The IUD: a protective alternative
Interestingly, research shows that the use of an intrauterine device (IUD) can actually have a protective effect. A meta-analysis of 16 studies involving more than 12,000 women showed that IUD use reduced the risk of cervical cancer by 33%.
The suspected mechanism is immune stimulation: the IUD causes a mild, chronic inflammatory response in the uterus, resulting in more immune cells being present that can recognize and clear HPV-infected cells.
Important for CIN 2/3
For women with CIN 2 or CIN 3 who have an IUD, it may be wise to consider removal of the IUD in some cases. This is due to progesterone receptor changes that can play a role in more severe abnormalities. This is always an individual decision in consultation with your practitioner.
lower risk of cervical cancer in women with an IUD, according to a meta-analysis of 16 studies with more than 12,000 women.
What can you do?
If you are HPV-positive and use the pill, there are several steps you can consider:
- Discuss alternatives with your GP: A copper IUD provides contraception without estrogen and may have a protective effect against cervical cancer.
- Optimize your estrogen metabolism: By eating cruciferous vegetables daily (broccoli, cauliflower, kale), you support the conversion toward the favorable 2-hydroxy-estrone pathway. DIM supplements can help with this.
- Strengthen your immune system: A strong immune system can partly compensate for the effect of estrogen on HPV. Focus on nutrition, supplements, and lifestyle.
- Get checked regularly: With long-term pill use and HPV, it is extra important to have a regular smear test and HPV test.
Personal advice on contraception and HPV
The choice of contraception is a personal decision. During the intake consultation, we will discuss which options best suit your situation and how we can optimize your estrogen metabolism.
Schedule an intake consultationVeelgestelde vragen
Should I stop the pill immediately if I have HPV?
Does the increased risk also apply to the mini-pill?
How does an IUD help against HPV?
How long after stopping the pill does the risk decrease?
Questions about your situation?
Feel free to get in touch for personal advice about your HPV diagnosis.
Contact us